
Understanding Cervical Cancer Through Maya and Zara’s Journey
The afternoon sunlight filtered through the café windows as Maya stirred her cappuccino absently, her mind clearly elsewhere. Across from her, Zara noticed the distant look in her best friend’s eyes and gently touched her hand.
“You’ve been quiet all week,” Zara said softly. “What’s going on?”
Maya looked up, her eyes glistening with unshed tears. “My cousin Amina was just diagnosed with cervical cancer. Stage three. She’s only thirty-two, Zara. Thirty-two.”
The words hung heavy in the air between them. Zara felt her heart constrict as she squeezed Maya’s hand tighter. “I’m so sorry. How is she doing?”
“She’s scared. We all are.” Maya took a shaky breath. “But you know what the worst part is? Her doctor said that cervical cancer is one of the most preventable cancers. If only she’d known about the HPV vaccine and regular screening, they might have caught it earlier.”
That conversation marked the beginning of a transformative journey for both young women, one that would lead them from fear and confusion to empowerment and advocacy.

The Wake-Up Call: Learning About Cervical Cancer
In the days following their conversation, Maya and Zara found themselves diving deep into research about cervical cancer etiology, prevention strategies, and early detection methods. What they discovered both alarmed and motivated them.
Cervical cancer develops in the cells lining the cervix, the lower part of the uterus that connects to the vagina. The primary culprit behind most cervical cancer cases is the human papillomavirus (HPV), a group of more than two hundred related viruses. Certain high-risk HPV strains, particularly HPV-16 and HPV-18, are responsible for approximately seventy percent of all cervical cancer cases worldwide.
“I had no idea HPV was so common,” Zara said one evening as they sat in Maya’s apartment, surrounded by medical journals and printouts from reputable health organizations. “It says here that nearly eighty percent of sexually active people will contract some form of HPV during their lifetime.”
Maya nodded, highlighting another passage in the article she was reading. “But here’s the thing—most HPV infections clear up on their own within two years. The problem occurs when persistent high-risk HPV infections remain untreated, potentially leading to precancerous lesions and eventually invasive cervical carcinoma.”
Understanding Risk Factors and Pathogenesis
As their knowledge deepened, the two friends began to understand the multifaceted nature of cervical cancer development. They learned that while HPV infection was the necessary cause, several cofactors could increase a woman’s vulnerability to developing the disease.
Immunosuppression emerged as a critical risk factor. Women with compromised immune systems—whether due to HIV infection, immunosuppressive medications, or other conditions—face significantly higher risks because their bodies struggle to clear persistent HPV infections effectively.
Smoking appeared repeatedly in their research as a modifiable risk factor. The carcinogenic compounds in tobacco can damage cervical cell DNA, making smokers twice as likely to develop cervical cancer compared to non-smokers with similar HPV exposure.
“Listen to this,” Maya said, reading from her laptop screen. “Long-term use of oral contraceptives for five years or more slightly increases cervical cancer risk, though the mechanism isn’t completely understood. But the research emphasizes that the cardiovascular and reproductive health benefits of contraception generally outweigh this small increased risk.”
Other risk factors included having multiple full-term pregnancies, early sexual activity before age eighteen, multiple sexual partners, and a family history of cervical cancer—all factors that could influence screening recommendations and prevention strategies.
The Power of Prevention: HPV Vaccination
The most revolutionary discovery in their research was the HPV vaccine, a powerful preventive tool that could eliminate up to ninety percent of cervical cancer cases if universally administered before HPV exposure.
Three vaccines currently protect against HPV infection: Gardasil 9, Gardasil, and Cervarix. Gardasil 9, the most comprehensive option, protects against nine HPV strains, including the seven high-risk types responsible for approximately ninety percent of cervical cancers and the two types that cause ninety percent of genital warts.
“The optimal vaccination schedule recommends administering the vaccine between ages nine and twelve, before any sexual activity begins,” Zara explained to Maya, who was taking notes. “But catch-up vaccination is recommended through age twenty-six, and even adults up to age forty-five can benefit after consulting with their healthcare provider.”
The vaccine typically requires two doses for those under fifteen years old, administered six to twelve months apart, while older adolescents and adults need three doses over a six-month period.
“I wish I’d known about this when I was younger,” Maya said quietly. “Amina probably didn’t even know the vaccine existed when she was the right age.”

Cervical Cancer Screening: The Second Line of Defense
While vaccination represented primary prevention, the friends learned that cervical cancer screening served as an equally crucial secondary prevention strategy, capable of detecting precancerous changes before they developed into invasive cancer.
Two main screening methodologies existed: the Papanicolaou test (Pap smear) and HPV DNA testing. The Pap test examines cervical cells under a microscope to identify abnormal cellular morphology, while HPV testing detects the presence of high-risk viral strains.
Current screening guidelines recommended that women begin cervical cancer screening at age twenty-one, regardless of sexual activity history. Between ages twenty-one and twenty-nine, Pap testing every three years was advised. For women aged thirty to sixty-five, three options existed: Pap testing alone every three years, HPV testing alone every five years, or co-testing with both methods every five years.
“The key message is that screening saves lives,” Maya emphasized, creating an infographic on her tablet. “Regular screening can reduce cervical cancer incidence by up to eighty percent because it catches precancerous lesions during the long window before they become cancerous—usually a process taking ten to twenty years.”

Recognizing Warning Signs and Symptoms
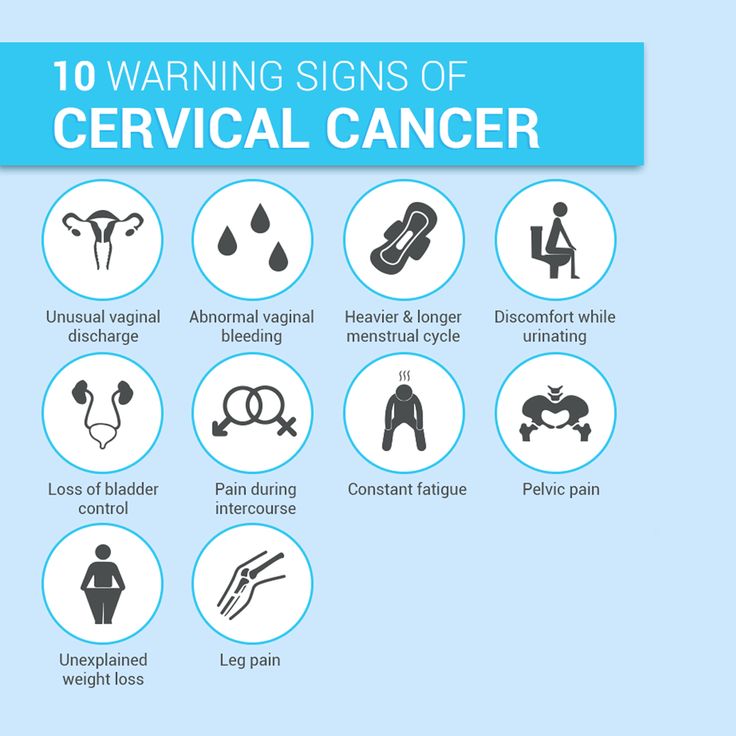
As their knowledge expanded, Maya and Zara learned to recognize potential cervical cancer symptoms, though they discovered that early-stage disease often presented asymptomatically—another reason why regular screening was so critical.
Advanced cervical cancer could manifest through several warning signs: abnormal vaginal bleeding between periods, after intercourse, or post-menopause; unusual vaginal discharge that might be watery, bloody, or foul-smelling; pelvic pain or discomfort during intercourse; and in advanced stages, symptoms like back pain, leg swelling, or urinary and bowel dysfunction.
“These symptoms can indicate many conditions besides cancer,” Zara noted, “but they should always prompt a visit to a healthcare provider for proper evaluation.”
Becoming Advocates: Their Mission Begins
Armed with comprehensive knowledge about cervical cancer epidemiology, prevention strategies, and screening guidelines, Maya and Zara decided to channel their concern into action. They couldn’t change Amina’s diagnosis, but they could help prevent other women from facing the same fate.
They started small, creating an Instagram account called “Silent Warriors” dedicated to cervical cancer awareness. They shared infographics about HPV vaccination, screening recommendations, and risk reduction strategies. They posted testimonials from survivors and explained complex medical concepts in accessible language.
Within weeks, their following grew exponentially. Young women from their community and beyond began sharing their own stories, asking questions, and thanking them for providing information that had never been adequately explained to them.
Maya and Zara organized community health workshops in collaboration with local gynecologists and oncologists. They visited schools to educate adolescent girls about the importance of HPV vaccination. They created multilingual resources to reach immigrant communities where cultural barriers often prevented open discussions about reproductive health.
“Knowledge is the most powerful weapon against this disease,” Zara would tell audiences at their workshops. “Cervical cancer doesn’t discriminate, but information and preventive healthcare can be the great equalizers.”
Broader Impact: Health Equity and Global Perspectives
As their advocacy work expanded, Maya and Zara became increasingly aware of healthcare disparities affecting cervical cancer outcomes. They learned that while cervical cancer incidence had declined dramatically in high-income countries with established screening programs, it remained a leading cause of cancer mortality among women in low and middle-income nations.
Geographic, socioeconomic, and racial disparities in access to vaccination, screening, and treatment contributed to these inequitable outcomes. Black women, Hispanic women, and those living in rural or underserved areas faced higher cervical cancer mortality rates despite the disease’s preventability.
This realization deepened their commitment to ensuring that accurate health information and resources reached all women, regardless of their circumstances.
Maya’s Personal Transformation
Six months into their advocacy journey, Maya accompanied Amina to one of her chemotherapy sessions. As they sat in the oncology center, surrounded by other patients fighting their own battles, Maya felt a profound shift in perspective.
“You know what you and Zara are doing is incredible, right?” Amina said, her voice weak but steady. “Every woman you educate, every girl who gets vaccinated because of your work—you’re saving lives.”
Tears streamed down Maya’s face. “I just wish I could have saved you from this.”
Amina smiled gently. “You can’t change my diagnosis, but you’re changing the future for countless others. That’s everything.”

A Call to Action
Today, Maya and Zara’s “Silent Warriors” initiative has reached thousands of women, facilitated hundreds of HPV vaccinations through community health partnerships, and helped countless women schedule their first cervical cancer screening appointments.
Their message remains clear and urgent: cervical cancer prevention is within every woman’s reach. Through HPV vaccination, regular screening, safe sexual practices, smoking cessation, and informed healthcare advocacy, women can dramatically reduce their risk of developing this once-common but now highly preventable disease.
As Maya often says at the conclusion of their workshops, “We’re all silent warriors in this fight—silent because cervical cancer often develops without symptoms, warriors because we refuse to let that silence claim more lives. Arm yourself with knowledge, protect yourself with prevention, and empower others with awareness. Together, we can make cervical cancer a disease of the past.”
The friendship between Maya and Zara, forged in shared experiences and strengthened by a common purpose, reminds us that personal tragedy can become a catalyst for positive change. Their story illustrates how education, prevention, and early detection can transform the landscape of cervical cancer from a devastating diagnosis to a preventable disease—one informed woman at a time.
- Must-Watch Movies Releasing in 2026: Your Complete Enterta1nment Calendar. - February 11, 2026
- World Tropical Diseases Day: The Silent Suffer1ng of 1.6b Lives. - January 31, 2026
- The El Molo Tribe: Kenya’s Last Fisher People Fight1ng for Survival on Lake Turkana’s Shores - January 30, 2026