Obesity is influenced by more than diet and exercise; the mind plays a powerful role in how our bodies gain and lose weight. It often begins in the brain, where stress, mood, and emotion shape the choices we make about food and activity.
Obesity is a condition where excess body fat builds up, increasing the risk of health problems like diabetes and heart disease. It results from a mix of lifestyle, genetics, and mental health factors that affect how the body stores and uses energy.
Obesity is a growing public health challenge with deep psychological roots. Globally, January marks Healthy Weight Awareness and Obesity Awareness Month, a time to reflect on the importance of maintaining a healthy weight not only for physical wellbeing but also for mental health.
In Kenya, rising rates of obesity and lifestyle diseases like diabetes, high blood pressure, and heart problems are becoming a serious concern, affecting both cities and rural areas. Looking at obesity from a mental health perspective shows why usual advice about diet and exercise often doesn’t work, and highlights how stress and emotions are closely linked to weight.
Recent trends illustrate just how desperate some individuals have become in the pursuit of weight loss. Globally and in Kenya, substances like Ozempic are being misused among fitness enthusiasts and young adults seeking rapid results, despite significant health risks and limited medical guidance. Extreme diets, detox teas, and unregulated weight-loss products are also on the rise, reflecting a pattern of quick fixes rather than sustainable change. These trends show the need for approaches based on evidence and psychology that support both mental health and healthy weight, making sure prevention and treatment are safe and effective.
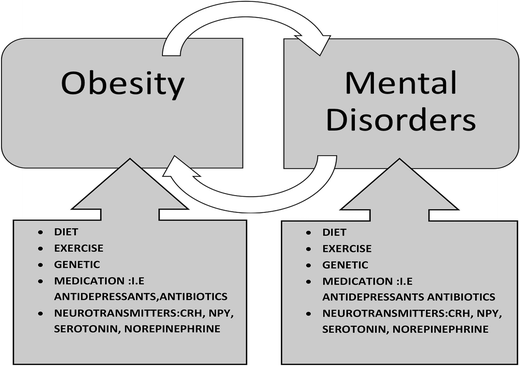
Obesity is about more than what we eat or how much we move. Our minds, how we handle stress, mood, and emotions, play a huge role in how our bodies gain or lose weight. Looking at obesity through this lens helps explain why quick fixes rarely work.
Obesity and Chronic Stress: The Brain’s Appetite Control Centers
Chronic stress doesn’t just make people feel tense or anxious, it actually changes how the brain responds to food signals in ways that promote weight gain. Research has shown that long‑term psychological stress can override normal satiety cues and interfere with the brain’s reward response, leading to stronger cravings for high‑fat and high‑sugar foods that provide quick emotional relief.
In a 2023 study from the Garvan Institute of Medical Research, scientists found in mouse models that chronic stress combined with calorie‑dense diets altered activity in the brain’s reward and appetite circuits, particularly in the lateral habenula. Under chronic stress, this region remained inactive, allowing continuous reward signals that encouraged eating even when the body was already full, and drove stronger preferences for sweet, highly palatable foods. These changes dampen the brain’s natural response to satiety, meaning that usual cues to stop eating become less effective under chronic stress.
Chronic stress triggers hormonal and brain changes that shift motivation toward high‑calorie foods and reduce the feeling of satisfaction after eating. The study Eating behavior and stress: a pathway to obesity highlights how these stress-driven changes in appetite and reward circuits can gradually increase the risk of weight gain and obesity.
Depression and Metabolic Flexibility
Depression does more than affect mood, it can also influence how the body uses energy at a fundamental level. Researchers have found that people with depressive symptoms tend to show higher levels of insulin resistance, a condition in which cells respond less effectively to insulin even when body weight is similar, suggesting a link between depression and dysregulated glucose metabolism. Meta‑analyses show that insulin resistance and other metabolic problems, like high fasting glucose, are more common in people experiencing depressive episodes, highlighting a biological link between mood and metabolism.
At the cellular level, depression is associated with impaired mitochondrial and energy metabolism, which affects the body’s ability to switch efficiently between burning carbohydrates and fats. Studies in neurobiology show that chronic depression can alter mitochondrial function and other pathways that regulate cellular energy production, leading to reduced metabolic flexibility, the capacity to adapt fuel use depending on availability and demand. This means that even when someone attempts weight loss through intentional changes, their physiology may resist these changes because energy regulation systems are already compromised.
The practical implication is that addressing depression can improve metabolic function and make weight management easier even without restrictive dieting, showing why mental health care should be part of comprehensive strategies for obesity prevention and treatment.
Executive Function Decline and Eating Behavior
Chronic stress does more than trigger cravings, it can impair the very brain functions that help us make healthy choices. The prefrontal cortex, responsible for planning, impulse control, and decision-making, becomes less effective under sustained psychological pressure. This means that even when people know what constitutes healthy eating and exercise, their brains may struggle to execute those intentions consistently. In other words, knowledge remains intact, but follow-through fails, creating a gap between understanding and behavior.
This cognitive overload directly affects obesity interventions. Programs that focus only on diet, exercise, or willpower often fail because they don’t consider how stress disrupts executive function. Non-adherence is frequently neurological rather than intentional, shifting the focus from blame to strategy. Effective approaches need to include stress management, emotional regulation, and mental health support alongside lifestyle guidance, highlighting why mental wellbeing is essential for sustainable weight management.
Emotional Eating as Mood Regulation
For many people under chronic stress or emotional strain, food becomes a reliable way to regulate mood. Palatable foods, those high in sugar, fat, or salt, trigger the release of dopamine and serotonin, creating a temporary sense of relief or pleasure. Unlike advice to “just relax” or “take a break,” eating provides an immediate, tangible effect on the brain’s reward system, which is why emotional eating often persists even when someone knows it may not be healthy. Research shows that these cycles of temporary relief are common and resemble other coping strategies, rather than constituting true addiction.
According to a 2021 systematic review and meta‑analysis on emotional eating and weight regulation, eating in response to emotions is a common behaviour linked with overweight and obesity, and interventions that address emotional eating can improve both emotional eating behaviours and modestly reduce weight.
Understanding emotional eating as a functional response rather than a moral failing changes how we approach obesity and mental health. The goal is not to shame or blame, but to identify alternative strategies that can fulfill the same emotional need safely. Mindful eating, stress management techniques, and emotional support can gradually replace food as the primary coping mechanism, helping individuals break the cycle while still acknowledging that eating for comfort is a natural, human behavior.
Rapid Weight Loss and Mental Health Destabilization
Rapid weight-loss strategies may seem appealing, but they can have unintended consequences for mental health. Severe caloric restriction and extreme dieting have been shown to increase irritability, anxiety, and depressive symptoms, often making it harder for individuals to sustain healthy behaviors. Hormonal changes that occur during aggressive weight loss can further disrupt mood regulation, leaving people more emotionally vulnerable and less able to cope with daily stressors.
A 2025 study published in BMJ Nutrition, Prevention & Health found that adults following calorie‑restrictive diets had higher scores for depressive symptoms compared with those not on a diet, particularly among men and people who were overweight. Researchers suggested that low‑calorie diets can lead to nutritional deficiencies and physiological stress that may worsen mood, fatigue, and other emotional symptoms.
These psychological effects also help explain why many people regain lost weight after restrictive dieting. Weight regain is often accompanied by heightened distress, frustration, and a sense of failure, creating a cycle that undermines long-term success. Research suggests that mental stability, rather than the speed of weight loss, is a stronger predictor of sustainable weight management, highlighting the importance of approaches that prioritize psychological wellbeing alongside physical goals. Understanding these links emphasizes that safe, gradual, and psychologically informed strategies are far more effective than rapid fixes.
Safe, Evidence-Based Approaches
Research shows that lifestyle programs that combine healthy eating, movement, and behavioural support can lead to meaningful improvements in weight and physical activity, even among people with mental health conditions. A large review of community and outpatient lifestyle interventions found that these kinds of programs were associated with modest but statistically significant reductions in weight and body mass index, as well as increases in physical activity and healthier eating behaviours like more vegetable intake. Studies in children and adolescents also show that structured lifestyle interventions can reduce symptoms of depression and improve quality of life, suggesting that supporting mental wellbeing alongside physical health can have dual benefits.
Obesity isn’t just about what you eat or how much you move. It’s tied up with how your brain handles stress, mood, and emotions. So often, what looks like “lack of willpower” is actually your brain trying to cope with pressure, anxiety, or emotional challenges. Understanding this changes the way we think about weight.
If we continue to treat obesity as a problem of discipline while ignoring the brain under stress, we will keep failing the very people we claim to help. The best approach is one that’s realistic, compassionate, and grounded in evidence, supporting mental health, building sustainable habits, and creating spaces where people can make changes that actually last. That’s how we help people win at both health and life.
- The Rise of Suicide Posts in Digital Spaces Reflects a Growing Mental Health Crisis - February 22, 2026
- How Kenya’s Silent Lifestyle Disease Crisis Is Reshaping Public Health - February 12, 2026
- The Rise of Lifestyle Diseases Emerges as a Crisis Among Kenya’s Youth - February 9, 2026

