Cervical cancer continues to impose a heavy burden on Kenyan women, and the silence surrounding its causes and prevention carries a high cost in lives lost and opportunities missed.
This January, recognized globally as Cervical Cancer Awareness Month, EpicPulse Magazine continues its health advocacy efforts in the fight against cervical cancer, raising awareness, promoting prevention, and amplifying the voices of those driving change.
According to the World Health Organization (WHO) fact sheet of December 2, 2025, cervical cancer is the fourth most common cancer among women globally, with around 660,000 new cases and approximately 350,000 deaths in 2022, the vast majority occurring in low- and middle-income countries due to inequities in prevention and care. In Kenya specifically, the most recent Ministry of Health reporting, drawing on GLOBOCAN 2022 data, records 5,845 new cervical cancer cases and 3,591 deaths annually, making it a leading cause of cancer death among women in the country.
In this discussion, silence refers to the cultural taboos, stigma, misinformation, and lack of open dialogue about reproductive health and cervical cancer prevention that together suppress awareness and discourage women from seeking early detection and vaccination. In Kenya and across sub‑Saharan Africa, research has consistently identified low levels of awareness and culturally rooted barriers as significant obstacles to uptake of cervical screening and HPV vaccination, key preventive measures.
Multiple studies have documented these barriers in Kenyan communities: for example, the qualitative research article “Barriers and Facilitators to Cervical Cancer Screening in Western Kenya: a Qualitative Study” (Journal of Cancer Education, 2021) found that fear of pain, embarrassment, low awareness of HPV/cervical cancer, and discomfort discussing reproductive health were significant obstacles to screening uptake among women and healthcare providers in Migori County. Similarly, the study “Developing a framework to describe stigma related to cervical cancer and HPV in western Kenya” (BMC Women’s Health, 2022) reported that discriminatory attitudes, assumptions about promiscuity or infidelity, and lack of clear understanding about HPV/cervical cancer contribute to anticipated and internalized stigma that reduces a woman’s likelihood of seeking screening or treatment services.
These findings align with broader systematic evidence (Barriers to cervical cancer screening in Africa) showing that negative beliefs and misconceptions, such as linking cervical cancer with immoral behavior or fearing that screening will harm fertility, lead many women to avoid discussions or services that could prevent the disease.
Why Silence Persists
Despite being preventable and well understood medically, silence about cervical cancer persists because of social, cultural, and systemic barriers that discourage open conversation and proactive prevention. In Kenya, research such as the qualitative study “Barriers and Facilitators to Cervical Cancer Screening in Western Kenya” found that low awareness of HPV and cervical cancer, fear of pain and embarrassment during pelvic exams, and a general discomfort discussing reproductive health are significant obstacles to women seeking screening. Participants in this study reported that both community members and healthcare providers struggled with knowledge and communication about the disease and preventive services, reinforcing avoidance rather than dialogue.
The persistence of silence is also linked to widespread misinformation and stigma. The systematic review “Barriers to Cervical Cancer Screening in Africa” highlights how myths about screening, including beliefs that it leads to loss of fertility, or that a speculum exam enlarges the vagina, deter women from utilizing services because they fear judgment from family and friends. Such misconceptions are compounded by cultural values emphasizing modesty and privacy, which make discussions about reproductive health taboo, especially in rural communities where these norms are strong. A Kenyan study “Socio‑cultural factors associated with the uptake of human papillomavirus vaccine among girls in Garissa County” (International Journal of Community Medicine and Public Health, 2025) showed that beliefs about vaccine side effects, infertility, and its association with promiscuity further suppress conversations about HPV vaccination among parents and guardians.
Importantly, silence around cervical cancer is not only a women’s issue; men’s attitudes and communication also affect prevention. Studies have identified that lack of male support or outright opposition to cervical screening and HPV vaccination can discourage women from seeking services, as decisions often require spousal approval or rely on household consensus. tematic evidence from African contexts notes that lack of male support for screening and negative community attitudes constrain women’s health‑seeking behavior.
Furthermore, rural–urban disparities highlight how stigma and silence disproportionately affect access. In urban areas, where media exposure and health campaigns are relatively stronger, public discussion and uptake of preventive practices have seen slow increases. In contrast, rural communities continue to face high levels of misinformation, fear‑based barriers, and moral judgments tied to sexuality, which limit access and discourage women from attending screenings or openly discussing HPV vaccination.
The Consequences of Silence
Silence around cervical cancer prevention contributes directly to late screening and delayed diagnosis, with devastating consequences. In Kenya, according to Human Papillomavirus and Related Diseases 2023 Report, cervical cancer continues to have one of the highest burdens of any female cancer, with more than 5,000 women diagnosed each year and over 3,200 deaths annually, making it the leading cause of cancer mortality among women.
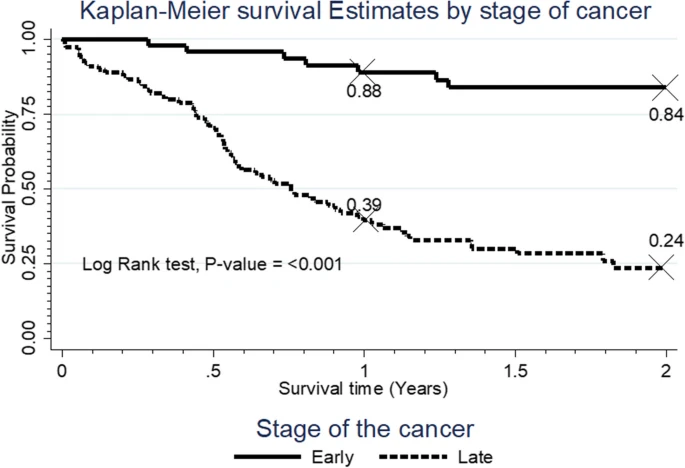
This high mortality is largely due to women being diagnosed at advanced stages, often when treatment options are limited and less effective.
When cervical cancer is detected too late, the human toll is devastating, with women and their families bearing the consequences. Studies in Kenya such as Survival of cervical cancer patients at Moi teaching and Referral Hospital, Eldoret in western Kenya indicate that more than 90 percent of women with cervical cancer are diagnosed at advanced stages, which is associated with significantly poorer outcomes. Survival probabilities also decline sharply with delayed diagnosis: research from Kenyan clinical settings shows that one‑year survival after diagnosis is around 57 percent, dropping to approximately 45 percent by two years without early intervention. By contrast, women whose cancer is detected early often have a much better chance of surviving, showing just how life-saving regular screening can be.
The emotional, financial, and public health burdens of late diagnosis ripple across families and communities. Women diagnosed at advanced stages face intense treatment regimens, higher medical costs, and prolonged periods away from work, placing significant stress on households that often lack health insurance or financial reserves. Beyond individual suffering, late‑stage disease exacerbates pressure on Kenya’s already strained health system, requiring more complex and expensive care compared with what would be needed for early‑stage cases. The combination of lost productivity, high treatment costs, and preventable deaths shows how silence around preventive health costs lives, deepening socioeconomic inequities.
Prevention and Awareness Efforts: Cervical Cancer in Kenya
Across Kenya, efforts to break the silence around cervical cancer prevention are gaining momentum through HPV vaccination campaigns, expanded screening services, and innovative community outreach. The Ministry of Health has intensified its commitment to early detection and vaccination, transitioning to a single‑dose HPV vaccination schedule that simplifies access and increases coverage among eligible girls aged 10–15, a step expected to protect significantly more young women with existing resources.
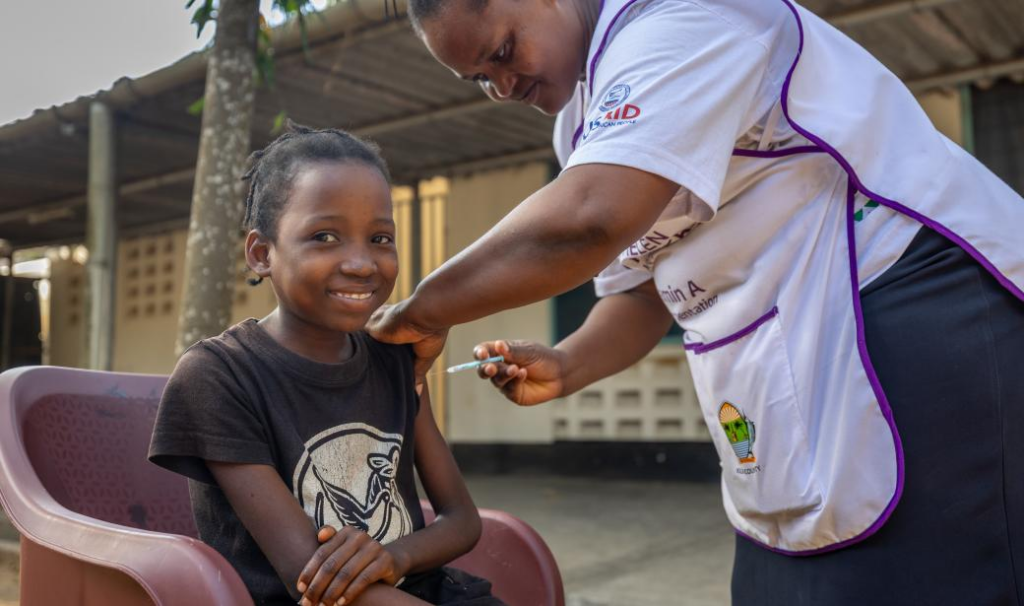
“Many girls were missing their second dose due to distance, costs, or forgetting to return, now, with just one visit, we can fully protect them against HPV.”
Kilifi County Nurse, Beatrice Dbwoge
This single-dose approach is helping more young girls access lifesaving protection against cervical cancer across Kenya.
At the community level, digital platforms like the AskNivi chatbot in coastal counties are helping women and families access reliable information on HPV vaccination and screening, linking users directly to clinics offering services and reaching tens of thousands of people with interactive education that dispels myths and encourages preventive action.
Community health workers, NGOs, and local clinics are also playing a central role in raising awareness and bringing services closer to women who face stigma, cost barriers, or limited mobility. Organizations such as NRHS Kenya have deployed mobile screening clinics and outreach teams, enabling thousands of women to receive visual inspection with acetic acid (VIA) and other screening tests in underserved regions, while training healthcare workers to improve the quality and accessibility of care.
Women, families, and community leaders can support prevention by starting conversations about vaccination and screening in homes and public spaces, sharing accurate information with peers, and actively seeking services at nearby health facilities; open dialogue and collective action remain powerful tools in overcoming silence and saving lives.
As we can see, this is a collective responsibility, each of us has a role to play in the fight against cervical cancer. While gaps in awareness and access remain, we can all contribute effectively, from advocacy and community education to reducing stigma. So, what are you doing?
Let’s all work together to make a difference in the fight against cervical cancer.
- The Rise of Suicide Posts in Digital Spaces Reflects a Growing Mental Health Crisis - February 22, 2026
- How Kenya’s Silent Lifestyle Disease Crisis Is Reshaping Public Health - February 12, 2026
- The Rise of Lifestyle Diseases Emerges as a Crisis Among Kenya’s Youth - February 9, 2026