Understanding the Lifeline for Kidney Failure Patients
What happens when your kidneys can no longer do their job? How does your body survive when its natural filters start to fail? For millions of people worldwide battling kidney disease, dialysis becomes a lifeline, literally replacing the function of their kidneys to remove waste and excess fluids. But not all dialysis treatments are the same.
Imagine your body as a well-oiled machine, with your kidneys working as its built-in filtration system. Now, picture what would happen if that system suddenly broke down, waste would accumulate, fluids would overflow, and the entire system would start to malfunction. This is exactly what happens when the kidneys fail. This is where dialysis steps in, acting as an artificial kidney to sustain life. There are two primary types: Hemodialysis Dialysis (HD) and Peritoneal Dialysis (PD), each with its own process, advantages, and challenges. Understanding these options can help patients and families make informed decisions about treatment.
The Role of the Kidneys
Your kidneys may be small about the size of a fist but their job is enormous. Every day, they filter around 50 gallons of blood, removing toxins, regulating blood pressure, and balancing essential minerals like sodium and potassium. Think of your kidneys as your body’s natural filtration system, working tirelessly to remove waste, regulate blood pressure, and balance electrolytes. They also help control fluid levels in the body, ensuring everything runs smoothly.
But when kidney disease progresses to the point of failure, often due to conditions like diabetes, hypertension, or genetic disorders, the body’s natural filtration system shuts down, leading to a dangerous buildup of toxins. As kidney function declines to less than 15% of normal capacity, waste and excess fluids accumulate, causing swelling, high blood pressure, shortness of breath, and life-threatening imbalances in the body’s chemistry. At this critical stage, medical intervention becomes essential to prevent severe complications and sustain life.
Dialysis as an Artificial Kidney
Dialysis is a medical process that mimics the function of healthy kidneys, filtering out waste, excess fluids, and toxins from the blood. Without it, patients with end-stage kidney disease (ESKD) would not survive. While dialysis is not a cure for kidney failure, it serves as a bridge, either sustaining life indefinitely or keeping patients stable while they await a kidney transplant, prolonging life and improving quality of living, allowing them to manage their condition..
There are two main types of dialysis:
1. Hemodialysis Dialysis (HD): Blood is filtered outside the body using a machine.
2. Peritoneal Dialysis (PD): A cleansing fluid is used inside the abdomen to filter waste naturally.
Hemodialysis Dialysis (HD)
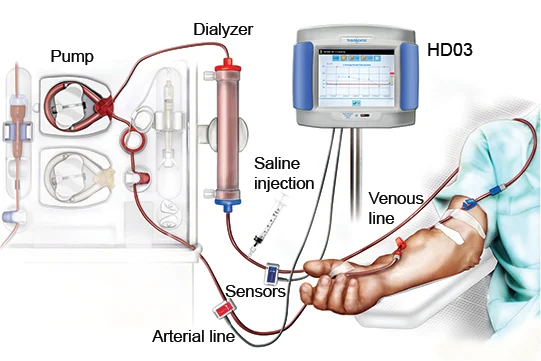
Think of hemodialysis as a high-tech washing machine for your blood. When your kidneys can’t filter out waste and excess fluids, hemodialysis steps in to do the job. The process involves drawing blood out of the body, cleaning it through a specialized filter called a dialyzer, and then returning the purified blood back into circulation.
The dialyzer, often called an “artificial kidney,” contains thousands of tiny fibers that act as a sieve, removing toxins and excess fluid while keeping essential blood components intact. Meanwhile, a special dialysis solution, known as dialysate, helps draw out harmful substances through a process called diffusion. After this thorough cleansing, the refreshed blood is returned to the body, helping maintain balance and prevent toxic buildup.
Where is Hemodialysis Done?
Hemodialysis can be performed in three main settings:
- In a hospital – Ideal for critically ill patients or those requiring intensive monitoring.
- At a dialysis center – The most common option, where patients visit a clinic 3 to 4 times a week for sessions lasting around 4 hours each.
- At home – With proper training, some patients opt for home hemodialysis, which offers more flexibility but requires commitment and medical support.
Each setting has its own trade-offs, with dialysis centers offering professional oversight, while home dialysis provides convenience and greater control over scheduling.
Access Points for Hemodialysis
Before dialysis can begin, doctors must create a safe and efficient way to access your bloodstream. This is one of the most critical aspects of hemodialysis. There are three main types of vascular access:
- Arteriovenous (AV) Fistula – Considered the gold standard, an AV fistula is created by connecting an artery to a vein in the arm, allowing for stronger blood flow. It lasts long and has a lower risk of infection.
- Central Venous Catheter (CVC) – Used in emergency or short-term dialysis, this involves placing a catheter in a large vein (often in the neck). While immediate and convenient, it has a high infection risk and is not a long-term solution.
- Arteriovenous (AV) Graft – If veins are too small or weak for a fistula, an AV graft (a synthetic tube) is implanted to connect an artery to a vein. It works well but has a higher risk of clotting.
The Hemodialysis Procedure: Step-by-Step
A typical hemodialysis session follows this process:
1. Preparation & Access – The patient is connected to the dialysis machine via the AV fistula, AV graft, or catheter. Blood pressure and weight are recorded to determine how much fluid needs to be removed.
2. Blood Filtration Begins – Blood is drawn from the body and passes through the dialyzer, where waste, excess fluid, and toxins are filtered out. The dialysate solution helps remove harmful substances while maintaining electrolyte balance.
3. Cleansed Blood Returns – Once purified, the blood is safely returned to the body.
4. Monitoring & Adjustments – Throughout the session, the machine continuously monitors blood flow, pressure, and composition to ensure the treatment is safe and effective.
5. Session Ends & Recovery – After 3 to 5 hours, the dialysis machine is disconnected, and patients may feel tired or lightheaded as their body adjusts. Some may experience muscle cramps or low blood pressure, but these symptoms typically fade over time.
Pros & Cons of Hemodialysis
Like any medical treatment, hemodialysis comes with both advantages and challenges.
Pros:
⦁ Highly effective in removing toxins and excess fluid.
⦁ Performed under medical supervision, ensuring safety.
⦁ Standardized treatment, with predictable outcomes.
Cons:
⦁ Requires frequent clinic visits, which can disrupt daily life.
⦁ Side effects such as fatigue, low blood pressure, and muscle cramps.
⦁ Dietary restrictions, including limits on fluid, potassium, and phosphorus intake.
Peritoneal Dialysis (PD)
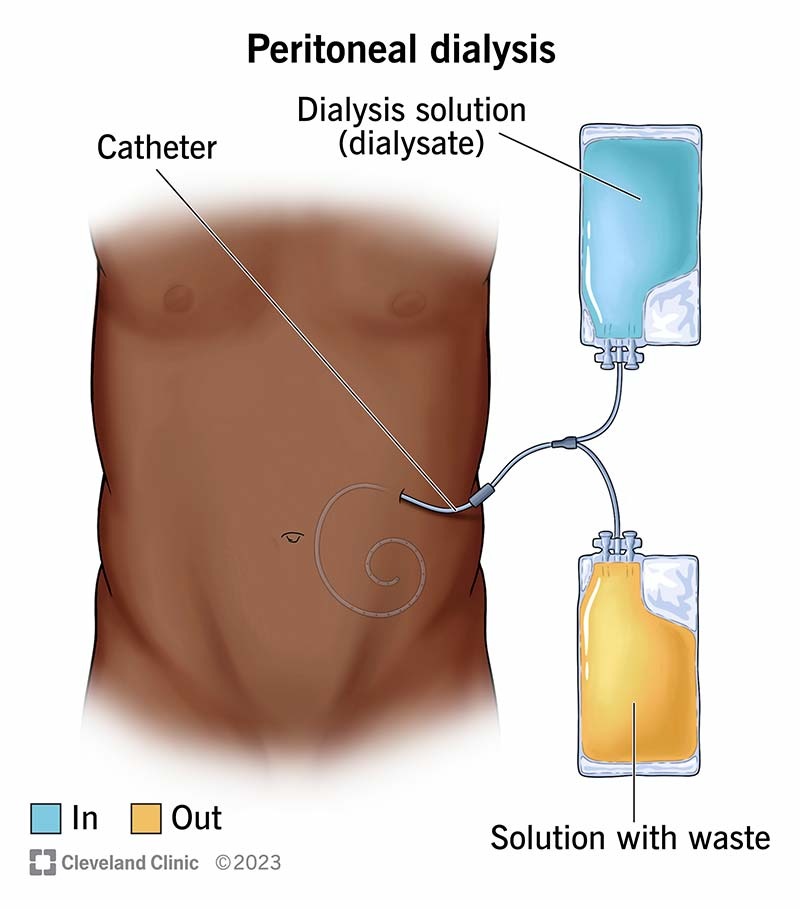
Imagine if your body could perform dialysis naturally – this is where peritoneal dialysis (PD) comes into play. Instead of relying on an external machine to filter your blood, PD uses the peritoneum, a natural membrane that lines your abdomen, as a filter.
In PD, a special solution called dialysate is introduced into the peritoneal cavity through a catheter. The peritoneum then acts like a filter, allowing waste products and excess fluids to pass from the blood vessels into the dialysate, which is then drained out and replaced with fresh solution. This process of filtering takes place inside your body, using your own tissue, making PD feel more natural and less mechanical than hemodialysis.
Types of Peritoneal Dialysis: CAPD vs. APD
i. Continuous Ambulatory Peritoneal Dialysis (CAPD)
This method is manual and typically requires 4-5 exchanges per day, where dialysate is infused into the abdomen and then drained, with the cycle repeating.
It’s done without the need for a machine, and the exchanges occur throughout the day, allowing patients to continue their daily activities during the filling and draining phases.
ii. Automated Peritoneal Dialysis (APD)
APD uses a machine to perform exchanges, typically overnight while the patient sleeps. The machine fills and drains the peritoneum with dialysate while the patient rests.
It requires fewer manual exchanges but still involves a nightly commitment.
The Peritoneal Dialysis Procedure: Step-by-Step
The steps for peritoneal dialysis are designed to be simple and adaptable to daily life. Here’s how it works:
- Catheter Placement – A catheter is surgically inserted into the peritoneal cavity, usually through the abdomen. It’s the key access point for dialysate infusion and waste drainage.
- Dialysate Infusion – The process begins when a sterile solution (dialysate) is infused into the peritoneal cavity through the catheter. The fluid is typically left in the abdomen for several hours to absorb waste and fluid from the bloodstream.
- Waste Removal – As the dialysate remains in the peritoneal cavity, it naturally draws out waste products, toxins, and excess fluids from the blood through the peritoneal membrane.
- Drainage Cycle – After a set amount of time, the used dialysate, now filled with waste, is drained from the abdomen through the catheter. Fresh dialysate is then infused to continue the process.
Pros & Cons of Peritoneal Dialysis
As with hemodialysis, peritoneal dialysis has its advantages and drawbacks, depending on your lifestyle, preferences, and health needs.
Pros:
⦁ More flexible than hemodialysis, as it can be done at home and at any time, including overnight with APD.
⦁ Fewer clinic visits compared to hemodialysis.
⦁ Because it’s more continuous, it tends to offer gentler fluid removal, reducing the likelihood of dramatic shifts in blood pressure or the feeling of being drained.
⦁ Ideal for active lifestyles since it doesn’t require time in a clinic during the day.
Cons:
⦁ Risk of infection, particularly peritonitis, which can occur if the catheter or the dialysate is not handled properly.
⦁ Requires commitment to daily care and hygiene.
⦁ The need for catheter care and exchanges may be cumbersome or uncomfortable for some people.
⦁ Space and cleanliness requirements are necessary for managing PD at home, as it involves careful storage of dialysis supplies and a sterile environment.
Peritoneal dialysis offers a flexible lifestyle with the freedom to move, travel, and sleep while undergoing treatment, making it an attractive option for many. However, the risk of infection and the physical demands of managing the process require that patients remain vigilant about hygiene and proper care.
Finding Hope Through Dialysis and Beyond
To patients and families living with dialysis, know that you are supported every step of the way on this journey. The road can be long and filled with challenges, but the advancements in dialysis treatments continue to improve, offering better outcomes, more flexibility, and enhanced quality of life. Whether it’s hemodialysis or peritoneal dialysis, each treatment option reflects human ingenuity and medical progress. With the right support, education, and care, managing dialysis can become part of a life that is still full of possibilities.
There is always hope. Medical science is evolving, and innovations continue to make treatments more accessible and effective, improving the lives of kidney failure patients every day. Hold on to hope, stay informed, and reach out for support when needed. With the right mindset and support network, it is possible to live a fulfilling life, even with the challenges that dialysis may bring. The journey might be tough, but your strength and the continuous advancements in kidney care serve as powerful reminders that brighter days lie ahead.
- The Rise of Suicide Posts in Digital Spaces Reflects a Growing Mental Health Crisis - February 22, 2026
- How Kenya’s Silent Lifestyle Disease Crisis Is Reshaping Public Health - February 12, 2026
- The Rise of Lifestyle Diseases Emerges as a Crisis Among Kenya’s Youth - February 9, 2026