Community health promoters in Kenya are emerging as a critical frontline force in the prevention of cervical cancer, bridging formal health systems and the communities they serve.
Bridging trust, health education, and service referral, these actors play an indispensable role in addressing persistent gaps in awareness, screening uptake, and early detection, particularly within underserved and hard-to-reach populations. As Kenya advances conversations on sexual and reproductive health and rights, the contribution of community-based healthcare practitioners remains central to translating policy and clinical interventions into meaningful, community-level impact.
In this feature, I was privileged to interview Phoebe Okore, a community health expert and sociologist with a strong commitment to community-based healthcare and sexual and reproductive health and rights, whose work spans community engagement, health promotion, and cervical cancer screening and prevention. She brings extensive experience across SRHR, adolescent sexual and reproductive health, integrated community case management, electronic community health information systems, and child health, and is currently pursuing a Master of Public Health with a focus on health promotion and international health.
Grounding Cervical Cancer Prevention in Community Health Practice
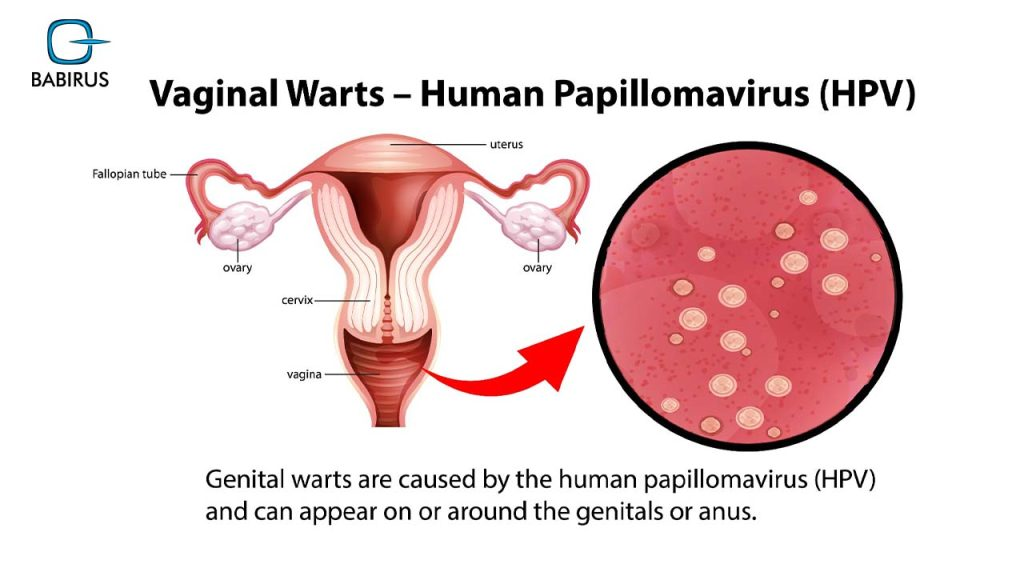
Community health promoters do more than deliver basic health services, they link knowledge, trust, and action within their communities. For issues like cervical cancer, which intersects both sexual and reproductive health (SRH) and mental health, their role is particularly critical. According to Phoebe Okore, a sociologist and community health expert, “Cervical cancer fits within the broader SRH because it affects the cervix, which is part of the female reproductive system, and its diagnosis can impact sexual health, relationships, and intimacy.”
She explains that the main cause of cervical cancer, the Human Papilloma Virus (HPV), is a common sexually transmitted infection, making prevention and education a central part of SRH efforts.
In Kenya, cervical cancer screening targets women aged 25–49, a group whose health priorities, reproductive health and non-communicable diseases such as breast and cervical cancer, overlap significantly. Beyond physical health, cervical cancer also affects mental wellbeing: “Diagnosis and treatment can lead to anxiety, fear, body changes, and societal stigma, all of which can affect a woman’s self-esteem and mental health,” Phoebe notes.
According to Kenya’s national cancer screening guidelines, women aged 25–49 are the primary target group for cervical cancer screening, underscoring the connection between reproductive health priorities and early detection strategies. Studies conducted in counties such as Kiambu have found that although awareness of cervical cancer is high, knowledge about HPV and screening remains limited and uptake of screening services is low, with many women describing the tests as costly, embarrassing, or painful. Research has also documented psychosocial barriers, including fear of abnormal results and stigma, that influence women’s screening behavior, highlighting how cervical cancer affects not only physical wellbeing but also emotional and social health.
Open discussions and health education in community forums not only reduce stigma but also empower women to make informed choices about their reproductive health, embrace HPV vaccination, participate in screening programs, and support those undergoing treatment.
Phoebe’s insights are shaped by hands-on research as well. Reflecting on her work in a cervical cancer study, she shares, “Most women hadn’t understood the importance of screening and had little to no information on HPV vaccination. Prevention also entails male involvement and addressing cultural barriers and misconceptions.” She highlights that making screening programs accessible and building trust with local leaders and community health promoters significantly improves uptake. These lessons continue to guide her approach today: education, accessibility, and community-led solutions are key to meaningful impact in cervical cancer prevention.
Barriers, Gaps, and Realities at the Community Level
While community health promoters play a critical role in cervical cancer prevention, their work is often challenged by persistent gaps in knowledge, cultural barriers, and structural constraints. Drawing on her experience in Kisumu, Migori and Siaya Counties, Phoebe Okore highlights some of the most common misconceptions around HPV vaccination and cervical cancer screening: “There is a misconception that having HPV means you already have cervical cancer. Some people don’t know that HPV actually causes cervical cancer, and others see it as just another STI.”
She also notes that fears around HPV vaccination such as concerns about infertility, severe side effects, or harm to young girls limit uptake. Some community members incorrectly view vaccination as a cure rather than a preventive measure, while many women prefer to wait for symptoms to appear before seeking screening, reflecting a mindset that “what you don’t know will not harm you.” Practical fears, such as apprehension about pelvic exams or Pap tests, along with uncertainty about who should be screened, where screening is available, and why it is important, further reduce participation.
Beyond knowledge gaps, social and cultural factors heavily influence women’s willingness to seek screening and treatment. Phoebe observes, “Stigma around cervical cancer, linking it to promiscuity or even believing it is a death sentence, discourages women from coming forward.” Gender dynamics also play a role: in many households, financial and healthcare decisions are controlled by men, who may limit women’s access to screening or treatment. Cultural norms regarding exposure to male healthcare providers further complicate matters, as many women are uncomfortable undergoing pelvic exams from men.
Additional challenges arise from women’s caregiving responsibilities, which often leave little time to prioritize their own health. Combined with limited access to accurate information, myths, and misconceptions, these factors create a landscape where cervical cancer prevention remains underutilized despite the efforts of community health promoters. Phoebe emphasizes that overcoming these barriers requires targeted education, culturally sensitive engagement, and trust-building between health workers and community members.
Vision for Community-Led Cervical Cancer Prevention
Addressing cervical cancer effectively requires both frontline action and innovative approaches that empower communities. For Phoebe Okore, frontline workers, including Community Health Promoters (CHPs), Community Health Assistants, nurses, and doctors, are central to strengthening prevention and referral pathways. She explains,
“Using mobile technology for education and awareness creation, CHPs can leverage eCHIS to pass key health promotion messages to women aged 25–49 on cervical cancer screening, and refer them to their linked health facilities for screening and management. This also applies to girls eligible for HPV vaccination.”
Phoebe Okore
Digital tools, she notes, are not only valuable for education and referrals but also for patient reminders, tracking appointments, and supporting diagnosis and treatment, providing real-time, verifiable data that makes follow-up easier.
This approach aligns closely with Kenya’s Community Health Policy 2020–2030, which emphasizes the role of community health workers in delivering preventive services, health promotion, and linking communities to formal health facilities.
By integrating digital tools like eCHIS into their work, CHPs operationalize the policy’s vision of a strengthened, data-driven community health system that improves access to care, ensures timely follow-up, and enhances the efficiency of health service delivery. The policy also prioritizes capacity-building, supervision, and support for community health actors, factors that are critical for sustaining initiatives like cervical cancer screening and HPV vaccination at the community level.
Community-driven approaches complement these technological solutions. Phoebe emphasizes the importance of empowering CHPs, who, as the most trusted level-one healthcare providers, can engage households directly, provide accurate health information, guide clients on HPV self-testing, and even assist in transporting samples to health facilities. She highlights the impact of community dialogues and action days, which create platforms to raise awareness, address fears and stigma, and dispel misconceptions. Additional strategies such as community health campaigns, roadshows, radio talk shows, and screen-and-treat outreach programs can further enhance education and screening uptake, particularly among underserved populations.
Looking to the future, Phoebe envisions a proactive, community-centered approach to cervical cancer prevention in Kenya.

“I see a community where CHPs are empowered to conduct pelvic exams such as VIA/VILI, guide women on HPV self-testing, and ensure all eligible girls receive HPV vaccination. Women will be informed, routinely screened, and those who test positive will receive timely treatment.”
Phoebe Okore
Through her current work, she actively contributes to this vision by facilitating community dialogues, mentorship sessions, and awareness campaigns aimed at dispelling myths and promoting cervical cancer prevention and HPV vaccination.
As we have seen, community health promoters play a significant role in cervical cancer prevention, and their impact could be even greater with the support of the wider community. Achieving meaningful change requires a collaborative approach, where healthcare providers, local leaders, policymakers, and community members all play their part in promoting awareness, encouraging timely screening, and ensuring access to care. Each of us has a role to play, whether it is sharing accurate information, supporting women to seek screening, or advocating for accessible services. What are you doing at a personal level to contribute to cervical cancer prevention, awareness, and timely care in your community?
- The Rise of Suicide Posts in Digital Spaces Reflects a Growing Mental Health Crisis - February 22, 2026
- How Kenya’s Silent Lifestyle Disease Crisis Is Reshaping Public Health - February 12, 2026
- The Rise of Lifestyle Diseases Emerges as a Crisis Among Kenya’s Youth - February 9, 2026