World AIDS Day, marked every December 1st, is one of those moments when the world collectively pauses to reflect on where we stand in the fight against HIV & AIDS.
It’s a day to honour the lives lost over the decades, to recognise the strength of people living with HIV, and to appreciate the families, health workers, activists, and communities who continue to carry this work on their shoulders.
We mark this day because HIV has not disappeared. New infections continue, stigma still pushes people into silence, and inequalities keep many from accessing prevention, treatment, and support. This day exists to remind us that the fight is ongoing, and that global attention is still needed.
In 2025, this reflection feels important than ever. The global theme, “Overcoming disruption, transforming the AIDS response,” speaks directly to the challenges shaping our reality today and the direction of the response moving forward. Conflicts have displaced families who rely on consistent treatment. Funding cuts are forcing frontline programs to scale down. Inequality is widening, making it even harder for vulnerable groups to access basic HIV services. Health systems, already stretched, struggle to keep prevention, testing, and treatment on track.
These disruptions slow progress and even create a real threat to the advances made over the years, particularly in prevention, treatment continuity, and community support.
The theme doesn’t end with the challenges, it points us toward what must be done. It calls for global solidarity at a time when the world feels increasingly divided. It demands human-rights-centred responses, ensuring that no one is denied care or dignity because of who they are or where they live. And it places communities at the centre of the response, recognising that lasting progress has always come from people on the ground, not just policies on paper. As we move toward the 2030 target of ending AIDS, 2025 stands as a defining year to recommit, rebuild, and act with the urgency this moment demands.
The Reality Through Numbers: Global, Africa, and Kenya
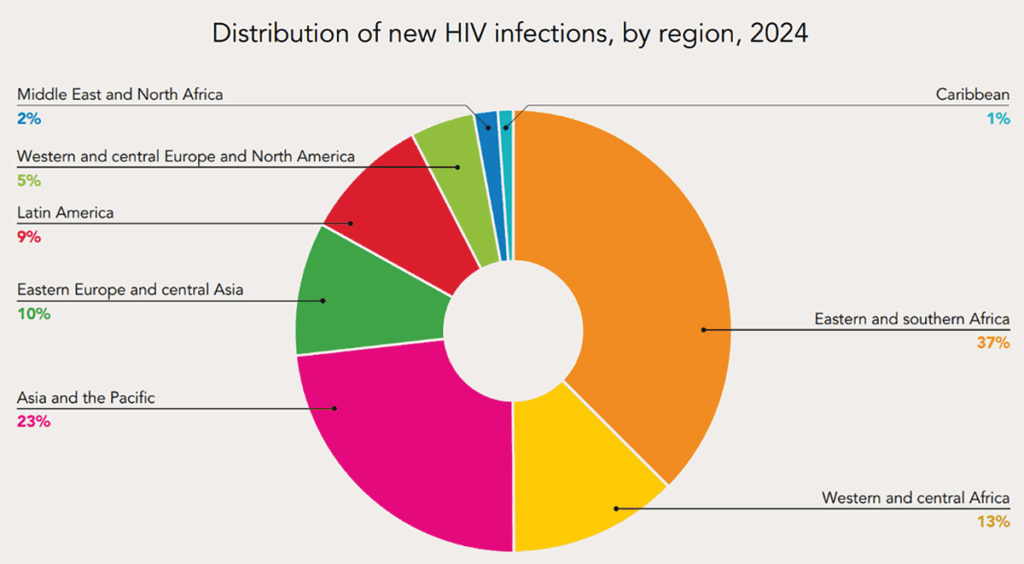
Globally, HIV remains a major public health challenge. According to the Global HIV & AIDS statistics Fact sheet by UNAIDS for 2024, about 40.8 million people were living with HIV worldwide. In that same year, 1.3 million people became newly infected. Tragically, about 630,000 people died from AIDS-related illnesses globally in 2024. Meanwhile, tens of millions receive antiretroviral therapy (ART), but coverage still falls short of global needs: in 2024 roughly 31.6 million people were accessing ART.
When we look at regional patterns, the situation becomes even more striking. According to a WHO July, 2025 Report, the World Health Organization (WHO) African Region remains the most affected. In 2024, the African Region accounted for roughly 65% of all people living with HIV worldwide, about 26.3 million individuals. The region also accounted for half of all new HIV infections globally in 2024.
In sub‑Saharan Africa (including East and Southern Africa), progress has been made: new HIV infections have fallen by 56% and AIDS‑related deaths by 59% since 2010. However, despite these gains, the burden remains massive, reflecting persistent inequalities in access to prevention, treatment, and social support. Adolescent girls and young women aged 15–24 years account for 28% of new HIV infections, highlighting their heightened vulnerability. Moreover, ongoing conflict, climate shocks, and displacement increasingly disrupt HIV services, threatening to reverse hard-won progress in the region.
The GBV-HIV Link in Women and Girls
There’s an ongoing campaign on the 16 Days of Activism Against Gender-Based Violence 2025, which underscores the urgent need to address the intersection of violence and health. Research shows that gender-based violence (GBV) contributes directly to higher HIV risk, particularly among adolescent girls and young women (AGYW) and adult women.
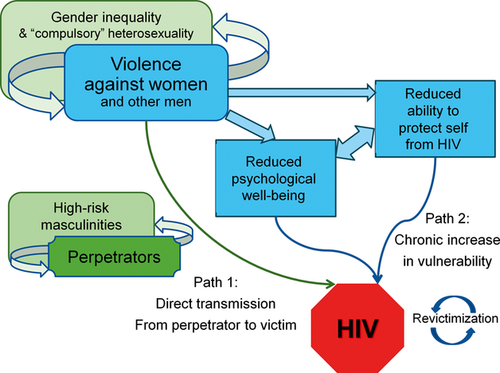
Physical, sexual, and psychological violence causes trauma and reduces access to HIV prevention, testing, and treatment services, leaving many women and girls more vulnerable in countries with high HIV prevalence. In 2024, women and girls accounted for 45% of all new HIV infections globally, including approximately 210,000 infections among AGYW aged 15–24, about 570 new infections per day. Globally, 4,000 AGYW acquired HIV each week, with 3,300 of these infections occurring in sub-Saharan Africa.
The campaign also highlights how systemic barriers and ongoing inequalities contribute to these risks. Many AGYW face overlapping challenges, including limited access to sexual and reproductive health services, social marginalization, and disrupted HIV programs. While 84% of pregnant and breastfeeding women living with HIV had access to antiretroviral treatment in 2024, progress has been slow, and gaps remain. Addressing HIV among women and girls therefore requires integrating GBV prevention and response into HIV programs, expanding access to services, and empowering women and girls to protect their health and futures.
Kenya In Focus
Turning to Kenya, the fight continues with mixed progress and ongoing challenges. According to recent national estimates, about 1.4 million Kenyans (adults and children) are living with HIV. Among adults (aged 15 and over), there are about 1.3 million people living with HIV. The national prevalence among adults 15–49 years has been reported around 3.2% in recent years. Encouragingly, Kenya has seen a steep decline in new infections: as of 2023, the number of new HIV infections was 16,752, down sharply from over 100,000 a decade earlier. Also, the number of people on ART has grown substantially; in 2023, over 1.33 million individuals were receiving treatment.
Despite progress in Kenya, serious gaps remain that threaten to slow the fight against HIV. So far in 2025, the country has recorded over 20,000 new HIV infections, bringing the total number of people living with HIV to approximately 1.33 million. While Kenya has made strides in testing and treatment, nearly 97% of people living with HIV know their status, and most of those are on antiretroviral therapy, treatment interruptions remain a major concern. In 2023 alone, over 41,000 people on ART stopped treatment, a worrying trend, because discontinuation increases risk of viral rebound and onward transmission.
Adding to the challenge, reports from early 2025 warned of potential shortages in key antiretroviral medications, threatening continuity of care for thousands more. Young people remain particularly vulnerable, and new infections in the 15–24 age group continue to be a concern. This combination of persistent new infections, treatment interruptions, and supply risks highlights that, even with progress, continued effort is vital to protect gains and advance the AIDS response.
Kenya’s 2025 World AIDS Day Commemoration


This year, the national commemoration for World AIDS Day (2025) was held on 30 November 2025 at Nyayo National Stadium in Nairobi, under the theme One Race, One Goal: Ending AIDS among Adolescents and Young People. The event included a national half‑marathon, youth‑centred medical camps, free testing, awareness campaigns, and community engagement, all aimed at expanding access to HIV prevention, testing, treatment, and support for young people.
The national leadership (including the Cabinet Secretary for Health) called on all Kenyans to rally in the fight against HIV/AIDS, stressing the need for sustained investment, equity in access to services (especially for youth), and community solidarity.
The 2025 commemoration offers an opportunity to reaffirm national commitment to the goal of ending AIDS by 2030, but the statistics and ongoing challenges remind us how far there is still to go.
Recent Global Setbacks Affecting the AIDS Response

In 2025, one of the most dramatic blows to the global HIV response has come from the sharp reduction in funding from the United States. When the US dismantled key foreign‑aid structures and sharply cut support for PEPFAR and other USAID‑backed HIV programs, the effect was immediate: prevention programmes shut down, community clinics closed, and supply chains for antiretroviral therapy (ART) and preventive tools were destabilized across many African countries.
A recent UNAIDS survey, ‘Impact of US Funding Cuts on Global AIDS Response’, found that nearly half of people living with HIV in East and Southern Africa experienced disruptions in treatment, and in some places, the provision of ART was reduced from the usual three‑to‑six‑month supply to far smaller quantities.
Even services aimed at high-risk and marginalized populations, such as adolescent girls and young women, sex workers, and LGBTQ+ communities, were among the first to suffer as drop-in centres and preventive programs were shut down.
These setbacks matter because they threaten decades of progress toward ending AIDS by 2030. With prevention efforts scaled back and treatment interrupted for hundreds of thousands, we risk seeing a resurgence in new infections and AIDS‑related deaths, especially among vulnerable groups like young people, women, and displaced or marginalized communities who already face barriers to care.
What had once been a clear global network of funding, clinics and community support structures is now fracturing under financial pressure, and unless new resources and political will are mobilized, many of the gains achieved across Africa over the last two decades could be lost.
Transforming the Response: What’s Working and What Must Change
Efforts to transform the HIV/AIDS response have shown that community leadership and grassroots initiatives are critical to making a real difference. Across Kenya, small community-based organizations, most founded and driven by people with lived experience in the sector, are filling gaps left by disrupted national programs, ensuring that prevention, treatment, and support reach the people who need it most. This grounding in lived experience allows their work to reflect the real needs of the communities they serve. These programs often focus on marginalized populations, including young people, women, and LGBTQ+ communities, who are most vulnerable to both infection and social exclusion.
5-Alive’s Community-Led HIV Response
One example of grassroots innovation is 5-Alive Development CBO, operating in Nakuru and Narok counties. The organization targets queer youths, female sex workers, young mothers, and other marginalized populations affected by HIV. By providing tailored services, ranging from peer support and counselling to direct access to treatment and prevention tools, 5-Alive ensures that even the most vulnerable have access to care. Its community-driven approach matters because it goes beyond treatment, building trust, social inclusion, and stronger engagement with care, which improve adherence and long-term health outcomes.
5-Alive’s impact is also reflected in the realities its leadership witnesses on the ground. Speaking on this year’s World AIDS Day theme, Founder and Executive Director Teddy Mwangi emphasized the urgency of protecting community-led services and sustaining an inclusive HIV response.

“The biggest disruptions we see are shrinking access to stigma-free, community-led services and rising inequalities caused by funding cuts. Kenya urgently needs sustained investment in grassroots, youth- and trans-led programs to keep the AIDS response resilient and inclusive.”
Teddy Mwangi, Founder, 5-Alive Development CBO
Another inspiring initiative is the Positive Young Women Voices (PYWV) Initiative, founded by Lucy Wanjiku Njenga. Registered as a community-based organization in 2017, PYWV addresses the specific challenges adolescent girls and young women face, particularly their heightened risk of HIV. Its programs include peer-to-peer mentorship, trainings for young men and women, LBQ support forums, and community outreaches. A flagship project, Adopt a Girl a Month, provides monthly mentorship, sanitary products, and life skills training, helping girls reduce their vulnerability to HIV while building confidence and agency. Through digital health tools, mental health support, and HIV-focused education, these youth-led, community-driven efforts are making a tangible impact on prevention, treatment awareness, and overall HIV outcomes for young women.
Aurelia Origi, Programs Officer at Positive Young Women Voices (PYWV), emphasized that strengthening Kenya’s AIDS response starts with putting more domestic resources into the health system, including reproductive health commodities, so the country isn’t overly dependent on external aid.
She stressed the need for investment in local manufacturing to secure access to life-saving medication and essential health supplies, alongside transparency and accountability to ensure resources actually reach the communities most affected. Aurelia also noted that policies must reflect the lived realities of the people they are meant to serve, and that meaningful impact can only happen when implementation matches intention.
“The only way the health sector can function effectively is if policies fit the lived realities of the people meant to be served, and are implemented to the letter.”
Aurelia Origi, Programs Officer, Positive Young Women Voices (PYWV)
Despite these successes, significant gaps remain. Health systems continue to struggle with shocks from funding cuts, conflicts, or pandemics, leaving treatment and prevention programs vulnerable. Greater investment is urgently needed to sustain HIV services, expand access to care, and improve prevention efforts. Stigma and discrimination still prevent many people, particularly adolescents, young adults, and marginalized groups, from seeking testing and treatment, highlighting the need for human-rights-centered policies and inclusive programs. Expanding access, ensuring continuity of care, and embedding equity at every level are vital steps if the HIV response is to be truly transformative and effective.
Advancing the Fight Against AIDS: Vision and Priorities

Protecting the progress made so far is the first step toward a stronger AIDS response. In Kenya, across Africa, and globally, sustained investment in HIV programs is needed to ensure they can withstand shocks from funding cuts, conflicts, or pandemics. Prioritizing youth engagement, supporting community-led initiatives, and expanding equitable access to prevention, testing, treatment, and mental health services will help close gaps and reach the populations most at risk. Strengthening strategies such as comprehensive education, PrEP, and community-based support is key to keeping the epidemic under control.
Looking toward 2030, a world where disruptions no longer derail health systems and the HIV response is inclusive, rights-based, and adaptable. Communities and health systems will be prepared to respond effectively to emerging challenges, while innovations in prevention and care continue to expand reach and impact. Ending AIDS will be a tangible reality, built on strong health systems, empowered communities, and sustained global commitment.
Achieving this vision depends on collective responsibility. Governments, communities, global partners, and individuals must work together to uphold the gains made, address ongoing inequities, and ensure that no one is left behind. By aligning action with vision, investing in sustainable programs, and centering the voices of those most affected, the world can turn the promise of ending AIDS into a shared achievement for all.
- The Rise of Suicide Posts in Digital Spaces Reflects a Growing Mental Health Crisis - February 22, 2026
- How Kenya’s Silent Lifestyle Disease Crisis Is Reshaping Public Health - February 12, 2026
- The Rise of Lifestyle Diseases Emerges as a Crisis Among Kenya’s Youth - February 9, 2026