Every year on November 12, the world comes together to mark World Pneumonia Day, a global call to action against one of the most preventable yet deadly infectious diseases. First established in 2009 by the Global Coalition Against Child Pneumonia, the day seeks to raise awareness, promote preventive care, and ensure that no life is lost to a disease that can be prevented, detected early, and effectively treated.
In 2025, the theme “Unite to Protect Every Breath” emphasizes the power of collective action in safeguarding health. . It highlights how governments, health organizations, and communities can work together to ensure access to clean air, good nutrition, and essential healthcare, key pillars in preventing and managing pneumonia. Supported by global health leaders such as WHO and UNICEF, this initiative continues to inspire worldwide efforts to reduce pneumonia-related deaths among both children and adults, reaffirming that protecting every breath means protecting every life.
Over the years, the day has evolved into a powerful campaign that unites governments, healthcare institutions, and civil society to advocate for improved vaccination coverage, oxygen availability, and stronger health systems.
Pneumonia remains one of the most pressing respiratory illnesses globally, claiming an especially heavy toll in children. According to UNICEF data, more than 700 ,000 children under the age of five die from pneumonia each year, equivalent to one child every 43 seconds.
Globally, there are about 1,400 pneumonia cases per 100,000 children under five annually, with incidence particularly high in West and Central Africa (≈1,620 per 100,000) and South Asia (≈2,500 per 100,000). Despite being largely preventable and treatable via vaccines, good nutrition, clean air and timely care, pneumonia continues to challenge health systems, especially in low- and middle-income countries.
In 2013, UNICEF and the World Health Organization launched the Integrated Global Action Plan for Pneumonia and Diarrhoea (GAPPD) under the banner “Ending Preventable Child Deaths from Pneumonia and Diarrhoea by 2025.” The plan set an ambitious target: reduce pneumonia deaths in children under five to fewer than 3 per 1,000 live births by 2025. Yet, despite progress in vaccination, treatment, and child health overall, many regions are still far from reaching that threshold. The persistence of large disparities in access to care, immunisation coverage and living conditions means that too many children continue to lose their lives to a disease that we know how to prevent and treat.
In Africa, the burden is even more acute. One review by African Journal of Current Medical Research estimated that pneumonia accounts for around 16 % of all deaths among children under five in sub-Saharan Africa, tying it with or surpassing other major causes of childhood mortality. While sub-Saharan African countries have made progress, the reductions in pneumonia mortality have lagged behind other childhood conditions.
For example, between 2000-2018 global pneumonia deaths among under-fives decreased by about 54 %, but the pace remains slow compared to diarrhoea or malaria. The interplay between malnutrition, air pollution, crowded living conditions and gaps in immunisation means that collective efforts are vital in the African context.
In Kenya, the challenge of pneumonia is acute and unevenly distributed. According to a national report, pneumonia causes between 8,000 and 10,000 childhood deaths annually, representing around one in five deaths among children under five. In terms of county-level mortality, for example, earlier data showed the under-five pneumonia mortality rate in some counties such as Mandera County at about 18 per 1,000 live births, while counties like Migori County and West Pokot County had roughly 15 per 1,000 live births, and several others ranging between 12-14 per 1,000.
Counties with stronger health systems and higher immunisation coverage, such as Nyeri and Kajiado, tend to have much lower mortality rates. These gaps highlight the urgent need for targeted action, improved access to healthcare, and stronger preventive measures to protect every child, regardless of where they live.
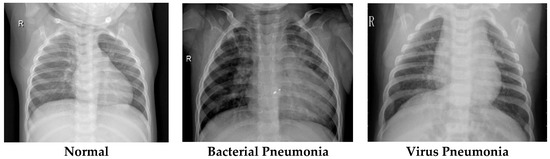
The respiratory illness can develop when infectious agents such as bacteria, virus, or fungi enter the lungs and trigger inflammation. The body’s immune system usually prevents such infections, but certain conditions or environmental factors can weaken these defences, making the lungs more vulnerable.
Viral pneumonia is caused by viruses such as influenza, respiratory syncytial virus (RSV), or coronaviruses. In some cases, antiviral medications, for example, oseltamivir for influenza or remdesivir for COVID-19, may be prescribed to reduce the severity and duration of illness. However, many viral pneumonias are mild and self-limiting, resolving on their own with rest, fluids, and symptom management.
Fungal pneumonia, on the other hand, requires antifungal medications such as fluconazole, itraconazole, or amphotericin B, depending on the type of fungus involved (e.g., Histoplasma, Cryptococcus, or Pneumocystis jirovecii). These medicines work by killing or inhibiting fungal growth to clear the infection.
Pneumonia is a treatable condition, and with timely medical care, most people recover fully. The treatment approach depends on the cause of the infection (bacteria, virus, fungi) its severity, and the patient’s overall health.
Some common treatment options for pneumonia include antibiotics, hospital care, antiviral medications, oxygen therapy, hydration and rest.
Antibiotics such as amoxicillin, azithromycin, doxycycline, or certain fluoroquinolones are commonly used to treat bacterial pneumonia, depending on the patient’s age, condition, and local resistance patterns. These medicines work by killing or inhibiting the growth of bacteria, allowing the lungs to heal. Most patients begin to feel better within 3 to 5 days, though recovery may take longer in severe cases. It is essential to complete the full prescribed antibiotic course, even if symptoms improve early, to prevent recurrence and the development of antibiotic resistance.
Most people begin to feel better within a week of treatment, though fatigue and mild cough may persist for some time. A complete pneumonia cure is possible when treatment is started early and followed consistently. Regular follow-up and lung evaluations are recommended to prevent long-term complications and ensure full respiratory recovery.
Preventing pneumonia begins with strengthening the body’s immunity and reducing exposure to infection-causing agents. Simple lifestyle habits, timely vaccination, and environmental precautions can go a long way in protecting both children and adults from this serious lung infection.
For children, breastfeeding, proper nutrition, and reducing indoor air pollution play a vital role in strengthening their natural defenses.
While pneumonia can affect anyone, certain groups are at a much higher risk of developing severe illness or complications. Understanding who is most vulnerable helps ensure that preventive care, vaccination, and early diagnosis reach those who need them most.
Groups at higher risk of the infection include young children under five years, older adults (above 65 years), people with chronic illnesses, immunocompromised individuals (whose immune system isn’t working properly). Malnourished individuals, people exposed to pollution and smoke and hospitalized or post-surgical patients are also at a higher risk of getting the infection.
Young children’s immune systems are still developing, making them more susceptible to infections like pneumonia. Their small airways can easily become obstructed, and they may not have received full vaccination protection.
Older adults (above 65 years) immune systems weaken with age, making it harder for them to fight off infections. Underlying health conditions, such as heart disease or diabetes, can further increase their risk of pneumonia.
Hospitalized patients are often exposed to more pathogens, and their immune systems may be weakened due to underlying health conditions or medical treatments. Invasive medical devices can also increase the risk of pneumonia.
The high vulnerability in these areas is linked to several interconnected factors such as poverty and living standards, limited access to healthcare, malnutrition and underlying health conditions, environmental factors such as poor living conditions, and inadequate vaccination coverage.
It can be challenging to distinguish pneumonia from other respiratory illnesses such as bronchitis, tuberculosis, or even heart failure, particularly in primary care settings where access to advanced diagnostic tools like chest X-rays or laboratory tests is limited. Identifying the exact cause, whether bacterial, viral, or fungal, is often difficult, which is why many patients receive empirical treatment based on clinical judgment before a definitive diagnosis is confirmed.
To improve patient outcomes, implementing validated severity assessment tools, such as the IDSA/ATS criteria, can help physicians triage patients more effectively and guide decisions on hospitalization and appropriate therapy. Enhanced access to point-of-care testing and chest X-rays further supports early and accurate diagnosis, enabling timely and targeted treatment. The IDSA/ATS criteria, developed by the Infectious Diseases Society of America and the American Thoracic Society, are a set of clinical guidelines that help doctors determine the severity of pneumonia and decide whether patients need hospital or intensive care.
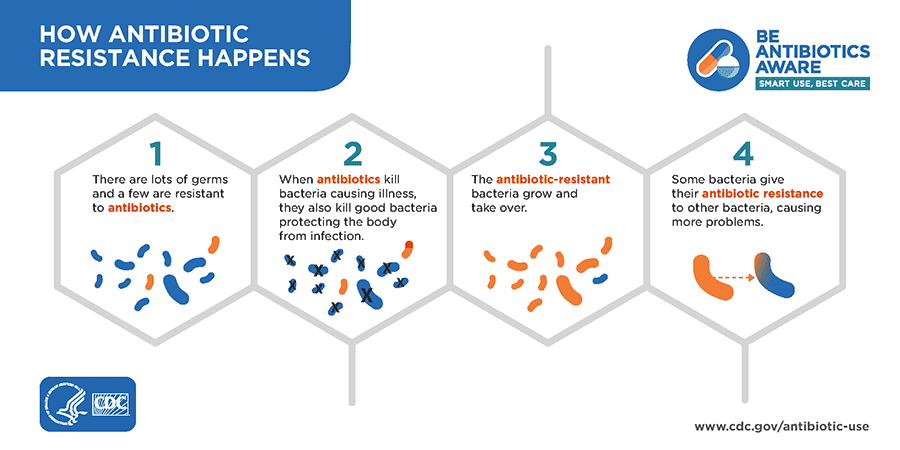
Rising Threat of Antibiotic Resistance
Pneumonia treatment faces challenges in accurate diagnosis, antibiotic resistance, and resource limitations, which can be addressed by improving diagnostic tools, practicing better antibiotic stewardship, and enhancing access to essential care like oxygen therapy and vaccinations.
The overuse and misuse of antibiotics, including taking them without prescription or failing to complete the full treatment course, has led to a worrying rise in antibiotic resistance. This means that common drugs become less effective against infections they once easily cured. As a result, illnesses such as pneumonia are becoming harder and more expensive to treat, particularly when caused by resistant bacteria like Methicillin-Resistant Staphylococcus aureus (MRSA).
According to the World Health Organization, antimicrobial resistance is among the top global health threats, with millions of deaths annually linked to resistant infections. Strengthening antibiotic stewardship, ensuring correct prescriptions, and promoting public awareness are essential steps in preserving the effectiveness of existing treatments.
Promoting the rational use of antibiotics, ensuring patients complete their full course of treatment, and developing new antibiotics are key strategies to combat antimicrobial resistance.
United Efforts to Fight Pneumonia
To reduce pneumonia cases, the government can increase funding for prevention and treatment programs, improve access to healthcare, and promote vaccination through awareness campaigns and policies.
Non-Governmental Organizations (NGOs) can raise awareness about pneumonia, support vaccination programs, provide healthcare services to vulnerable populations, and advocate for policy changes that prioritize pneumonia prevention and treatment.
Collaboration between the government, NGOs, and the public is essential in the fight against pneumonia. By working together, these stakeholders can ensure that pneumonia prevention and treatment efforts are comprehensive and effective.
The public can take proactive steps by getting vaccinated, practicing good hygiene, breastfeeding and providing good nutrition to children, avoiding smoking and indoor air pollution, and seeking medical attention promptly if symptoms arise.
Preventing pneumonia requires a combination of healthy habits and protective measures. Vaccination against pneumococcal bacteria, Hib, and influenza is one of the most effective ways to reduce risk, especially for children and older adults. Maintaining good hygiene, such as regular handwashing and covering coughs or sneezes, helps limit the spread of germs.
Reducing exposure to tobacco smoke and polluted air protects the lungs, while a balanced diet, adequate hydration, regular exercise, and sufficient sleep strengthen overall immunity. Managing chronic health conditions like asthma, diabetes, or heart disease also lowers the risk, and avoiding close contact with people who are sick further helps prevent infection.

As we mark World Pneumonia Day 2025, it’s clear that we all have a role to play in the fight against this preventable disease.
So, what part will you play in protecting every breath?
Through these collective efforts, we can reduce the incidence of pneumonia and improve health outcomes for individuals and communities worldwide.
Written by Charity Shitote, Editorial Intern at EpicPulse Magazine.
- The Rise of Suicide Posts in Digital Spaces Reflects a Growing Mental Health Crisis - February 22, 2026
- How Kenya’s Silent Lifestyle Disease Crisis Is Reshaping Public Health - February 12, 2026
- The Rise of Lifestyle Diseases Emerges as a Crisis Among Kenya’s Youth - February 9, 2026