Every year on October 10, the world comes together to mark World Mental Health Day, a moment to reflect, learn, and act on the state of mental well-being globally.
The 2025 theme “Mental Health in Humanitarian Emergencies” shines a light on the often-overlooked psychological toll of crises such as conflicts, natural disasters, and displacement. It reminds us that amid the urgency to provide food, shelter, and safety, mental health must not be left behind.

In this feature, I, Carson Anekeya, will be expounding on this theme, why this year calls for more than awareness. It’s high time we rethink our approach to humanitarian response, one that protects both bodies and minds.
When Humanity is Tested
When disasters strike, our first instinct is to save lives, erect shelters, and distribute food and water. Yet amid the urgency and flurry of physical rescue, another crisis often unfolds in silence, the toll on human minds.

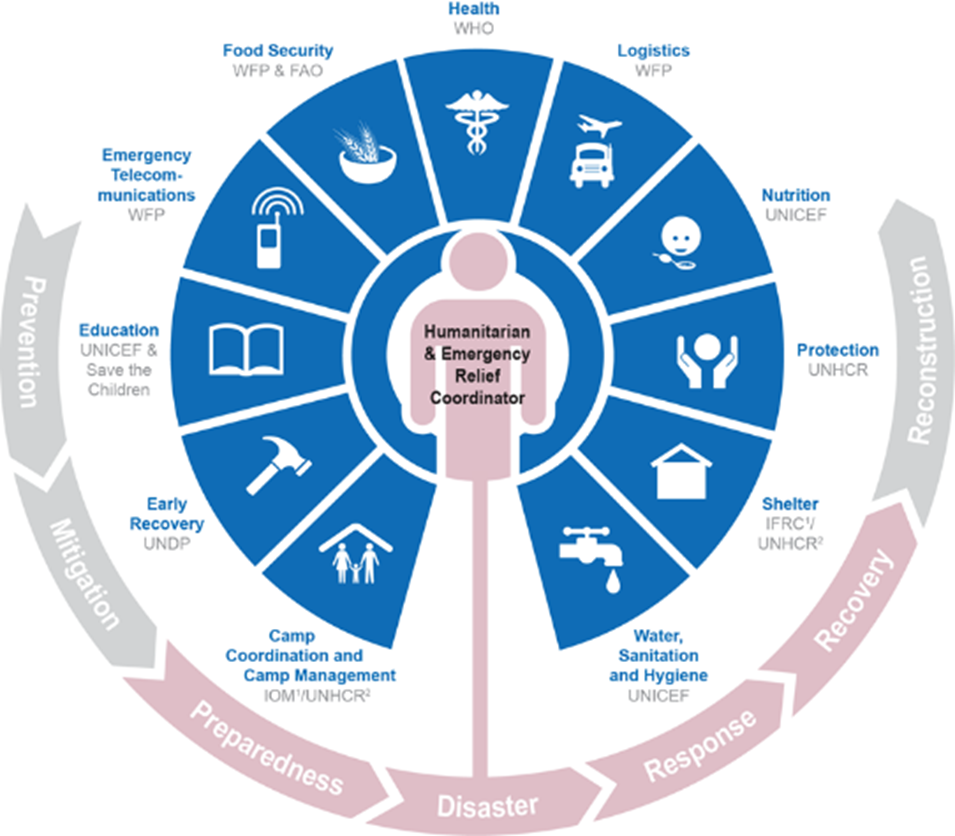
A humanitarian emergency as defined by Humanitarian Coalition refers to an event or series of events, such as armed conflict, natural disasters, epidemics or mass displacement, that poses a critical threat to the health, safety, security, or well-being of a population, often exceeding the capacity of local systems to cope. In such emergencies, the immediate focus is on survival: food, water, shelter, and physical safety. But crises carry wounds that cannot be seen: trauma, grief, fear, loss, and uncertainty multiply as lives are broken, uprooted, and reshaped. In these situations, vulnerability becomes a defining factor, shaping who suffers most, who recovers, and who is left behind.
Vulnerability refers to the reduced capacity of individuals or groups to anticipate, cope with, resist, and recover from the impact of hazards, a condition often rooted in poverty and social inequality. Poor populations are more likely to be severely affected by disasters and recover more slowly. Within affected communities, vulnerable groups such as children, pregnant and nursing women, persons with disabilities, migrants, and displaced people face heightened risks. Humanitarian crises generally fall under three main types: natural disasters, man-made emergencies, and complex emergencies. Each of these intensifies existing vulnerabilities in different ways, often disrupting livelihoods, displacing populations, and straining both physical and mental health.
In Kenya and across Africa, we have witnessed floods, prolonged droughts, internal conflicts, displacement and pandemics, each leaving psychological scars long after the physical reconstruction begins. According to findings from the World Bank Blogs, 41% of refugees and 29% of host-community members in Kenya report experiencing at least mild symptoms of depression or anxiety in recent weeks.
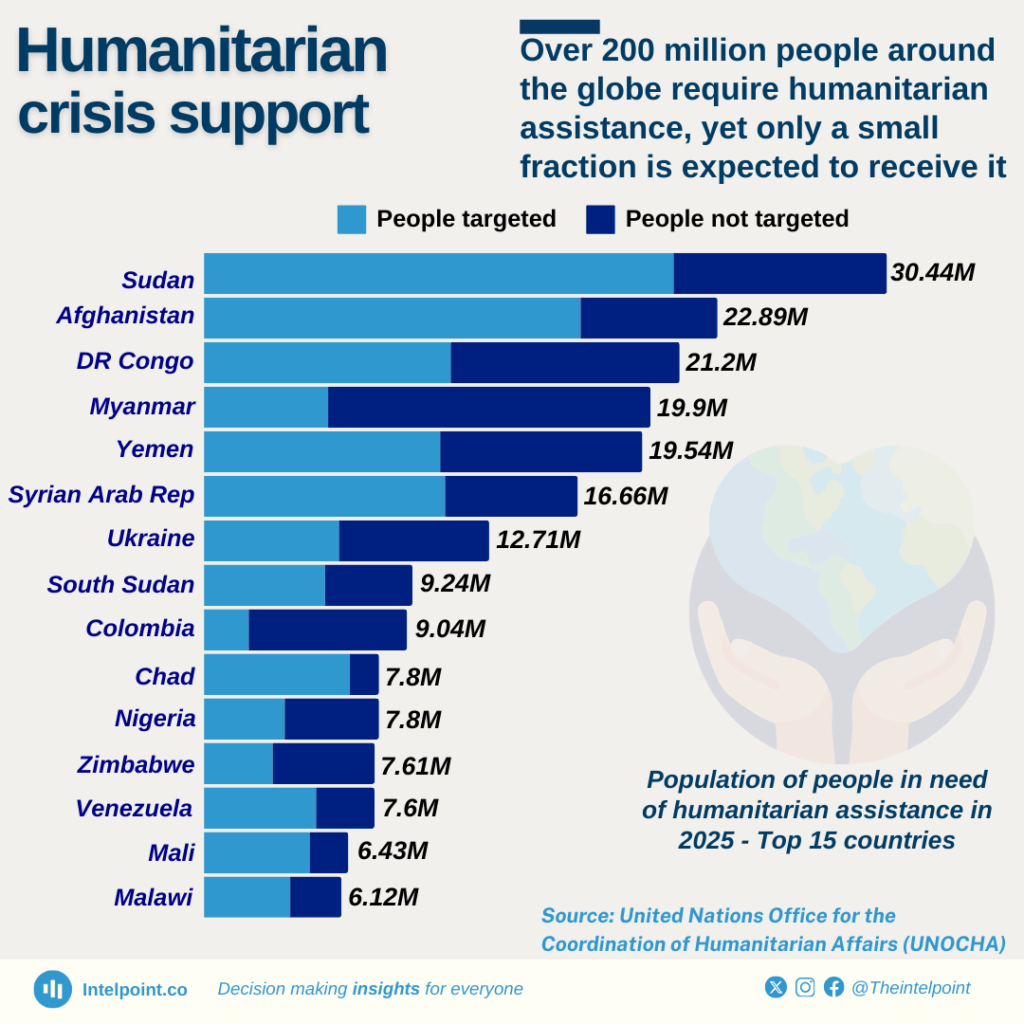
According to UN News and the World Health Organization (WHO), nearly one in five people (about 22%) affected by crisis settings may develop a mental health condition such as depression, anxiety, post-traumatic stress disorder, bipolar disorder, or schizophrenia. Meanwhile, about 9% of conflict-affected populations live with moderate to severe mental disorders that significantly impair daily functioning.
The Overlooked Emergency — Mental Health in Times of Crisis
In every humanitarian emergency, the visible damage, destroyed homes, collapsed infrastructure, and displaced families, often overshadows an invisible one: the erosion of mental well-being. Amid the chaos of survival, psychological wounds run deep, yet they receive far less attention than physical needs. Fear, grief, uncertainty, and loss silently take root, affecting individuals’ capacity to recover and rebuild their lives. This gap makes mental health one of the most overlooked emergencies within global humanitarian response.
Humanitarian crises strip individuals not only of safety and stability but also of control and connection, two pillars essential for psychological resilience. For many survivors, trauma is not a single event; it’s a prolonged state of uncertainty. Displacement, loss of loved ones, food insecurity, and violence often lead to chronic stress that lingers long after physical wounds heal. According to the study “Psychiatric Disorders in Refugees and Internally Displaced Persons After Forced Displacement: A Systematic Review,” displaced populations, especially refugees and internally displaced persons (IDPs), face heightened risks of anxiety, depression, and post-traumatic stress due to exposure to violence and the disruption of social networks.
The impact is even deeper among vulnerable groups. Women and children, who make up the majority of displaced populations, often face compounded trauma, from sexual violence and exploitation to family separation and poverty. Aid workers, too, carry invisible burdens. Studies show high rates of burnout, secondary traumatic stress (STS), and compassion fatigue among humanitarian workers: for example, a meta-analysis of nine studies with 3,619 aid workers found that rates of burnout ranged from 8.5% to 32%, depression from 10.4% to 39.0%, anxiety from 3.8% to 38.5%, and PTSD up to 25%.
Neglecting mental health in these contexts doesn’t just harm individuals, it slows entire communities’ recovery. Without psychosocial support, trauma can translate into cycles of violence, hopelessness, and mistrust. And when we talk about mental health in humanitarian emergencies, we must recognize that it’s not only about those affected by crisis but also about the humanitarian aid workers themselves.
Prolonged exposure to suffering, loss, and instability takes a psychological toll on responders, leading to burnout, secondary trauma, and compassion fatigue. If those offering help are emotionally overwhelmed, their capacity to support others diminishes. Mental health in humanitarian settings is therefore a two-way concern, everyone matters.
Reimagining Humanitarian Response
To truly respond to humanitarian emergencies, we must move beyond the idea of survival toward one of wholeness. While food, water, and shelter remain essential, so too are empathy, connection, and psychological care. A reimagined humanitarian response is one that recognizes mental health as a pillar of recovery, not a privilege to be addressed later.
Integrating psychosocial support into every stage of crisis response must become a global standard. This means training emergency responders, health workers, and community leaders to recognize signs of psychological distress and provide trauma-informed care. Community healing spaces, where survivors can share their stories, grieve together, and regain a sense of belonging, have been shown to accelerate recovery. Programs like Stand Out 4 Mental Health that combine art, play, and group therapy also provide safe ways for children and adults to process their emotions, rebuilding hope from within.
Globally, organizations such as WHO, UNHCR, and Médecins Sans Frontières (MSF) have made strides in embedding mental health care into humanitarian interventions. In Kenya, it is high time grassroots movements and community-based initiatives embraced the integration of mental health into humanitarian response. We witness disasters and crises unfold around us almost daily, from floods and fires to conflicts and displacement. Addressing mental well-being should not be left solely to large organizations like the Red Cross. Real change begins when communities take ownership, when we choose to care for one another before waiting for outside help.
And when I talk of humanitarian programs, I’m not only referring to large-scale interventions led by global organizations. Every responder, from volunteers and teachers to community leaders and journalists, plays a role in shaping the mental health outcomes of affected populations. This is why mental health literacy and psychosocial preparedness should be part of every humanitarian worker’s foundation, regardless of their professional background.
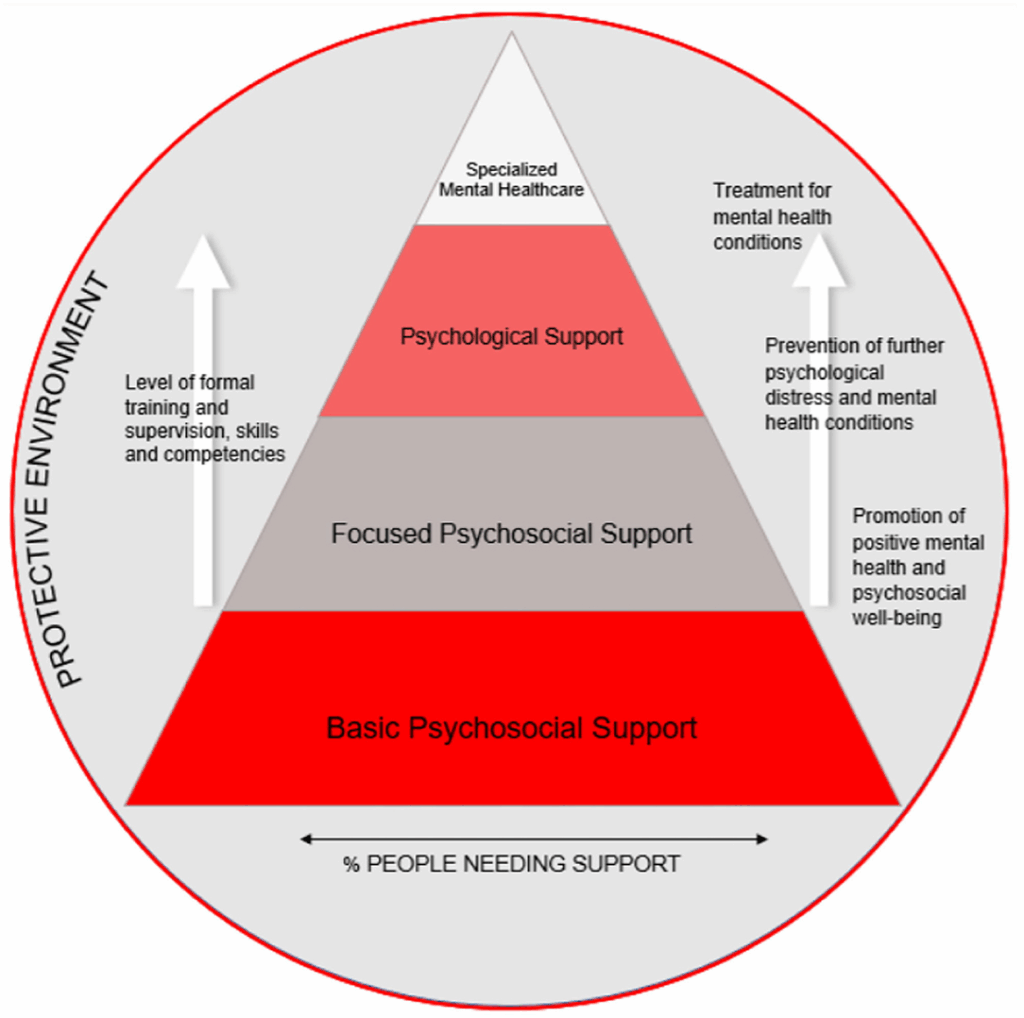
Everyone can begin this journey through the Foundations of Mental Health and Psychosocial Support (MHPSS) course, an online, self-directed certification developed by the MHPSS Collaborative, the Humanitarian Leadership Academy, and Save the Children. It’s a great starting point for anyone seeking to understand how to respond compassionately and effectively in crisis settings. The course introduces key MHPSS concepts, terminology, and the continuum of care, including the layers of the IASC MHPSS Pyramid of Intervention and Psychological First Aid (PFA) principles, practical tools that strengthen both individual and collective capacity to support mental health in humanitarian contexts. You can access the course here.
Reimagining humanitarian aid through the lens of mental health restores something more than infrastructure, it restores dignity. Helping people survive is not enough; when we also help them feel and hope again, we begin the real work of rebuilding. True humanitarianism begins where compassion meets care, in seeing people not only as victims of crisis but as humans capable of recovery and renewal.
Building a Compassionate Future
As the world continues to grapple with conflicts, climate disasters, and displacement, it becomes clear that rebuilding homes without healing hearts is an incomplete response. Mental health must be seen as life-saving, not supplementary, not optional, but essential. Policymakers, humanitarian agencies, and community leaders must integrate mental health services into every phase of crisis response, from preparedness to recovery. Every emergency plan should acknowledge that trauma, fear, and grief are as real as hunger or injury.
True humanity lies not only in the ability to provide shelter and safety, but in our willingness to listen, to comfort, and to walk beside those whose worlds have fallen apart. Supporting mental health in humanitarian settings is about preserving dignity, ensuring that those affected by crises are not just survivors, but humans capable of rebuilding meaning and hope. And as we mark World Mental Health Day 2025, I hope we begin to embody this truth, this year and in the years to come, evolving into a world where compassion is not conditional, and mental well-being stands at the heart of every humanitarian response.


“When humanity is tested, compassion must lead, for it is only through healing the unseen wounds that we prove our shared humanity.”
Carson Anekeya
As mental health advocates, we must continue to raise our voices, educate communities, and influence systems so that care and compassion are no longer the missing pieces in humanitarian response. The future we build depends on the empathy we extend today, to the displaced mother, the grieving child, the frontline worker, and even to ourselves.
- The Rise of Suicide Posts in Digital Spaces Reflects a Growing Mental Health Crisis - February 22, 2026
- How Kenya’s Silent Lifestyle Disease Crisis Is Reshaping Public Health - February 12, 2026
- The Rise of Lifestyle Diseases Emerges as a Crisis Among Kenya’s Youth - February 9, 2026